The NIMH funded the Multimodal Treatment of Attention Deficit Hyperactivity Disorder (MTA) study. It was a study of several treatments for almost 500 children with ADHD, including
- medication only
- medication and therapy combined
- therapy and community support, without medication
The study spanned many sites, and entailed collecting follow-up data for several years (read more).
The One Year Results
In 2007, Jensen and a team of researchers (Jensen et al., 2007) explain that the 14 month results of the study showed the following:
- Those treated with medication (either medication alone or a combination of medication and therapy) showed significant gains, based on teacher ratings of social skills, parent ratings of the parent-child relationship, and achievement tests of reading skills.
- Of note, 90% of those prescribed medications took them at least half the time by the 14 month mark. Given that many medications are meant to be given two or three times a day, this would mean that some children received their morning dose but did not take their afternoon dose, or skipped medication several days a week.
- Where the child had a combination of ADHD and an anxiety or behavior disorder, therapy and medication was better than medication alone.
This seemed to indicate that medication was the most effective treatment, and thus should become the standard treatment for ADHD.
The Three Year Results
At 36 months, the results seemed to have changed:
- All children diagnosed with only ADHD showed about the same improvement, regardless of the treatment they received. The initial differences between those who took medication compared to those who did not seemed to have disappeared. That is to say, at 14 months, those children prescribed medication clearly showed better adjustment and functioning than those who did not. However, by three years, those who took medication and those who did not seemed the same.
- Those children with Conduct Disorder, Oppositional Defiant Disorder, or a depressive disorder, however, showed fewer treatment gains, regardless of which treatment they received. Further, those with ongoing educational struggles continued to experience these struggles.
This has caused a great deal of debate:
- Some argued that if all treatments have the same outcome at three years, then children can wait either three years or just 14 months to experience significant benefits of treatment. Since medication had a significant benefit at 14 months, medication is the fastest way to see improvements for ADHD children. As a result, medication is the best treatment for ADHD children.
- Others argued that if all treatments have the same outcome at three years, then medication might offer a quick initial gain, but the long-term view shows that the other options are just as good. They noted that the children’s educational struggles continued unchanged while they were on medication, and those children with other disorders made less progress regardless of taking medication. Thus, a long-term view would better serve these children. As a result, they concluded medication is not the best treatment for ADHD children.
How could researchers and experts draw two completely different conclusions from the same study?
- Part of the problem is the focus. The short-term view is different than the long-term view.
- Part of the problem is the change in the groups. At the three year point, about half the children in the medication-only group had stopped taking medication, and about half of the children in the therapy-only group had started taking medication. Thus, about half the children in the study switched groups.
This is a serious problem. Imagine for a moment that you are a researcher testing a new treatment for some health issue, and you believe it is better than the standard treatment:
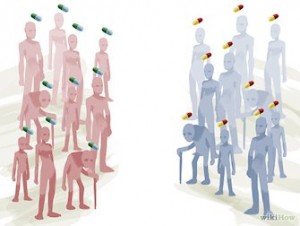 First, you would get a large sample of similar people with the health issue, and divide them evenly into two groups. You would be careful to make sure the groups were the same size and had similar people. You would check to make sure they were similar in terms of their gender (you had the same number of men and women in the groups), age range (you had the same number of younger, middle-age, and older people in the groups), and health status (you had the same number of severe, moderate, and mild cases in the groups). Once you were sure they were similar, you would continue with the study.
First, you would get a large sample of similar people with the health issue, and divide them evenly into two groups. You would be careful to make sure the groups were the same size and had similar people. You would check to make sure they were similar in terms of their gender (you had the same number of men and women in the groups), age range (you had the same number of younger, middle-age, and older people in the groups), and health status (you had the same number of severe, moderate, and mild cases in the groups). Once you were sure they were similar, you would continue with the study. - Next, you would provide your new treatment to the first group (the experimental group). You would provide the standard treatment to the second group (the control group).
- At the end of the study, you would look to see whether there were any differences in the outcomes for the groups.
What might you find?
- Suppose that at the end of the study you find the control group is unchanged (or maybe a little worse). However, the health status for the experimental group is much better. What would explain this difference? You look closer and see there are fewer cases of severe and moderate health problems, more cases of mild health problems, and some people who do not have the health problem at all anymore. It seems most everyone got better. Chances are… if the only starting difference between the groups was the new treatment, then the cause of the ending difference is the new treatment. You probably would conclude that the new treatment is better than the standard treatment (and be very happy to find this).
- Suppose that at the end of the study you find the control group is unchanged (or maybe a little worse). However, the experimental group is a little bit healthier. What would explain this difference? You look closer and see there are no cases of people without the problem, and no change in the number of mild cases. However, there are more moderate cases and fewer severe cases. It seems the new treatment helped people, but only those people who had severe cases. Again, chances are… if the only starting difference between the groups was the new treatment, then the cause of the ending difference is the new treatment. You probably would conclude that the new treatment helped (and be happy to find this).
Alternately… suppose that at the end of the study there was no difference in health status between the two groups. What would explain this?
- Suppose you looked closer and saw that the two groups had the same number of severe, moderate, and mild cases. Chances are… if the groups started and ended being very similar to each other, then the new treatment made no difference.
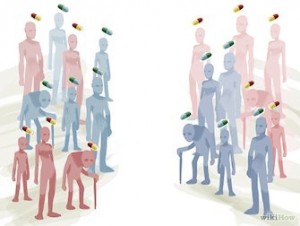 However, suppose you looked closer and saw that half the people in the two groups switched places. Half the people receiving the new treatment stopped it and started receiving the standard treatment, and half the people receiving the standard treatment stopped it and started receiving the new treatment.
However, suppose you looked closer and saw that half the people in the two groups switched places. Half the people receiving the new treatment stopped it and started receiving the standard treatment, and half the people receiving the standard treatment stopped it and started receiving the new treatment.
This would be a problem.
- You might think you could straighten this out by moving the groups back to the way you had them at the start of the study. However, this would not help. It would be hard to tell whether one treatment was better, as half of each group received some of the other treatment. It would be hard to tell whether the treatments were equally effective, as half of each group only got some of the treatment. In other words, for both groups, half the people in the group should not be there.
- You might think you could straighten this out by making three groups. The first group would be the people who started the new treatment and stayed with it. The second group would be the people who started the standard treatment and stayed with it. The third group would be the people who changed groups. This would solve the problem with the first and second group, but it would introduce a new problem for the third group. The people in this group would be very different, as they were exposed to four different treatments. Suppose:
- Some received the new treatment for a while, stopped and received no treatment, and then started the standard treatment.
- Some received the new treatment for a while, stopped it, but quickly started the standard treatment.
- Others received the standard treatment for a while, stopped it, but quickly started the new treatment.
- Others received the standard treatment for a while, stopped and received no treatment, and then started the new treatment.
- You might think you could straighten this out by simply throwing out the data for all the people who switched groups. That way, all the people in the experimental group received all of the new treatment, and all of the people in the control group received all of the standard treatment. There would be no “mixed” group. This would fix the problem… but would create at least two new problems:
- By throwing out data for half the sample, you have a much smaller number of people being treated. As a result, you have a much smaller chance of determining whether the new treatment is any better than the standard one.
- By throwing out data for half the sample, you lose a great deal of information about the treatment. For example, suppose the people who stopped the new treatment decided to do this because it was making their condition worse. You wouldn’t know about these cases where the treatment failed because you threw out the data for those people.
Thus, having half the sample switch groups is a serious problem… and there really is no way to fix it.
This is what happened in the MTA study. At the three year point, half the children in the study switched groups. As a result, half the people in the medication group only took medication for part of the study, and half the people in the no-medication group actually did take medication during the study. We can’t know which treatment led to better outcomes, or whether they were different at all.
The Eight Year Results
In 2009, Molina and a team of researchers published a follow-up study (Molina et al., 2009), and reported on the results of these children/teens (over 400 stayed in the study) after six to eight years.
They found, overall, that all children with ADHD (regardless of the type of treatment they received) continued to show lower adjustment than non-ADHD peers from the community. For example,
- ADHD teens overall performed about a half of a standard deviation below their non-ADHD peers. They had lower grade-point averages (2.75 vs 3.02) and were more likely to be held back a year in school (37.3% vs. 17.9%).
- Only 40% of ADHD teens had their driver’s license when they became eligible, compared to 58% of community teens.
- Arrests were more common among ADHD teens (39%) than the community sample (14%).
- Psychiatric hospitalizations were more common among ADHD teens (10%) than the community sample (1%).
You might be wondering about the children who took medication compared to those who didn’t. As explained above, remember that this comparison was confusing because children switched groups. At the six to eight year mark, even more of the children/teens had switched groups, so the number who never took medication was rather small.
Nonetheless, they found that the children/teens fell into three groups:
- Class 1 (34% of the sample) – These would be the children who started in the medication group and continued taking medication. They showed a good initial response to medication, continued improvement on medication over the first three years, and continued benefits from medication six to eight years later. For example, they showed significantly better achievement scores in math after six to eight years, compared to ADHD teens who did not take medication or who took and then stopped medication. They also were generally the only teens receiving ADHD treatment at the six to eight year mark.
- Class 2 (52% of the sample) – These would be most of the children who switched groups. They showed good improvements initially with medication, and maintained these gains over time. Of note, these children showed less severe problems at the start of the study, as well as better social adjustment, SES and family stability, and intelligence test scores. Over time, they discontinued medication (even the ones who started to take it in the middle of the study), as well as therapy and other treatments (even the ones who started therapy in the middle of the study) altogether. Those who received both medication and therapy needed slightly fewer school services, compared to those who had received only therapy.
- Class 3 (14% of the sample) – These would be a few of the children/teens who switched groups, and the few children/teens who never took medication. They seemed to show some immediate improvements at the start of their treatment (whatever treatment they received), but these improvements faded. By six to eight years, all had stopped receiving any treatment.
The authors provide a few points they believe can clearly be concluded from the study:
- Medication seemed very helpful to about a third of ADHD children, and somewhat helpful to about half the ADHD children. Thus, taking medication, even if only for only part of the six to eight year period, seems to have helped most children in the study (34% in Class 1 plus 52% in Class 2 equals 86% helped by at least some use of medication).
- However, all the ADHD children were still behind their peers in academic and social development by the time they reached adolescence. Thus, while medication was helpful, it did not erase the effects of ADHD.
- Only a small number of children continued to take medications into adolescence. Thus, we might press more teens to continue taking medication. However, even those who did still take the medication as teens fell behind their peers in terms of academic and social development. Recall that ADHD often occurs with learning disabilities as well as other problems. The long-term effect of ADHD (and other problems when present) continue, regardless of treatment with medication alone, both medication and therapy, or therapy alone. (However, see the upcoming post on ADHD and driving).
In short, they conclude that asking “Is medication better?” is not really important. What is important is that our most effective treatments do not really resolve the problems associated with ADHD.
ADHD, Medication, and Achievement
The findings of the MTA Study are consistent with those of other studies.
For example, Powers et al (2008) followed 90 ADHD children for nine years, and compared them to a diverse sample of 80 non-ADHD children. They examined
- scores on the WIAT (an achievement test, or test of school-based learning)
- scores on the WISC (an IQ test, or test of general intelligence)
- high school grade-point average and grade retentions
Of note, most of the medicated group had been taking medications consistently for 5 years. They found several interesting things:
- Generally, non-ADHD children had the highest scores, unmedicated ADHD children had the lowest scores, and the difference between these groups was statistically significant.
- ADHD children treated with stimulants obtained scores that fell between the other two groups:
- They were 5 points lower than non-ADHD children on math, but 4 points higher than unmedicated ADHD children.
- They were 6 points lower than non-ADHD children on reading, but 3 points higher than unmedicated ADHD children.
- Unmedicated ADHD children fell further behind each year. This was especially the case with reading scores, but also with math scores when the ADHD symptoms were more severe.
The authors note that the numbers vary, but conservative estimates indicate 20-25% of ADHD children also are diagnosed with a learning disorder. Thus, medication likely helps with the ADHD symptoms, but could not be expected to completely close the achievement gap because medication could not compensate for a learning disability.
- The same pattern was shown for general intelligence scores and grade-point average:
- Non-ADHD children scored on average 96 (where 100 is average) on the general intelligence test, and their grade-point average fell in the middle of the C range.
- Medicated ADHD children scored on average 95 on the general intelligence test, and their grade-point average fell in the low C range.
- Unmedicated ADHD children scored on average 90 on the general intelligence test, and their grade-point average fell in the middle of the D range.
- A little over 20% of non-ADHD children repeated a grade, compared to 25% of medicated ADHD children, and 25% of unmedicated ADHD children. Thus, ADHD children (medicated or not) appear slightly more likely to repeat a grade.
Thus, medication does help and improve the achievement scores and grades of ADHD children (as medicated ADHD children scored higher than non-medicated ADHD children), which likely does improve general intelligence scores. However, medication does not completely remove the effects of ADHD.
References
Jensen, P. S., Arnold, L. E., Swanson, J. M., Vitiello, B., Abikoff, H. B., Greenhill, L. L, Hechtman, L., Hinshaw, S. P., Pelham, W. E., Wells, K. C., Conners, C. K., Elliott, G. R., Epstein, J. N., Hoza, B., March, J. S., Molina, B. S., Newcorn, J. H., Severe, J. B., Wigal, T., Gibbons, R. D., Hur, K., (2007). 3-year follow-up of the NIMH MTA study. Journal of the American Academy of Child and Adolescent Psychiatry, 46, 989–1002.
Molina, B. S., Hinshaw, S. P., Swanson, J. M., et al. The MTA at 8 years: Prospective follow-up of children treated for combined-type ADHD in a multisite study. Journal of American Academy of Child and Adolescent Psychiatry, 48(5), 484–500.
Powers, R. L., Marks, D. J., Miller, C. J., Newcorn, J.H., & Halperin, J. M., (2008). Stimulant treatment in children with Attention-Deficit/Hyperactivity Disorder moderates adolescent academic outcome. Journal of Child and Adolescent Psychopharmacology, 18(5), 449–459.
